What Is a Baby Called That Died Right Before Birth
How common are large babies?
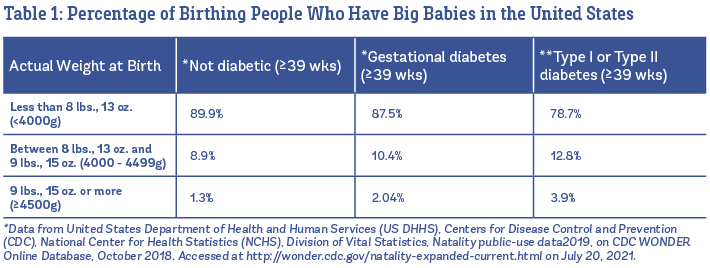
About one in x babies is born big in the United States (U.Southward.). Overall, 8.9% of all babies built-in at 39 weeks or afterwards weigh between 8 lbs., thirteen oz., and nine lbs., 15 oz., and 1.three% are born weighing ix lbs., 15 oz. or more (U.S. Vital Statistics, 2019). In Table 1, you lot can run into the percentages listed separately babies born to people who are not diabetic, vs. babies built-in to those with gestational diabetes and Type I or Blazon Two diabetes.
What factors are linked to having big babies? Big babies run in families (this is influenced past genetics), and it's more common to have a big baby when the babe's sex is male (Araujo Júnior et al. 2017). As yous can see in Table one, people with diabetes before or during pregnancy take college rates of big babies compared to people who are non-diabetic. Other factors that are linked to large babies include having a higher body mass index (BMI) before pregnancy, college weight proceeds during pregnancy, older age, post term pregnancy, and a history of having a large baby (Araujo Júnior et al. 2017; Rui-Xue et al. 2019; Fang Fang et al. 2019).
Among people with gestational diabetes, researchers have found that having a higher blood saccharide at commencement diagnosis makes you more likely to accept a baby who is large for gestational age. (Metzger et al. 2008). However, pregnant people who manage their gestational diabetes through diet, practice, or medication can bring down their chances of having a big baby to normal levels (or about 7%) (Landon et al. 2009).
In improver, at that place is high quality testify from 15 randomized trials showing that significant parents who exercise (both those with and without diabetes) have a significant decrease in the compared to those who exercise not practise during pregnancy (Davenport et al. 2018).
What is routine care for suspected large babies?
The nigh detailed bear witness we have on typical treat large babies comes from the U.S. Listening to Mothers Three Survey, which was published in the early 2010s. Although only one in x babies is built-in large, researchers found that 2 out of three families in the U.Southward. had an ultrasound at the end of pregnancy to decide their baby'south size, and one out of iii families in the study were told that their babies were also large. In the finish, the average birth weight of their suspected "big babies" was only 7 lbs., 13 oz. (Declercq, Sakala et al. 2013).
Of the people who were told that their baby was getting big, two out of three said their care provider discussed inducing labor considering of the suspected large infant, and one out of 3 said their care provider talked well-nigh planning a Cesarean because of the big baby.
Most of the families whose care providers talked most induction for large baby ended up being medically induced (67%), and the rest tried to self-induce labor with natural methods (37%). Almost 1 in 5 survey respondents said they were non offered a choice when it came to induction—in other words, they were told that they must be induced for their suspected big babe.
When intendance providers brought upward planning a Cesarean for a suspected big infant, one in three families ended up having a planned Cesarean. Two out of five survey respondents said that the discussion was framed as if at that place were no other options—that they must have a Cesarean for their suspected big babe.
In the end, care provider concerns about a suspected large infant were the fourth almost common reason for an induction (making up sixteen% of all inductions), and the fifth most common reason for a Cesarean (making up 9% of all Cesareans). More than half of all birthing people (57%) believed that an consecration was medically necessary if a care provider suspects a big infant.
So, in the U.South., most people have an ultrasound at the end of pregnancy to estimate the baby'south size, and if the baby appears large, their intendance provider will usually recommend either an consecration or an elective Cesarean. Is this approach evidence-based?
This approach is based on five major assumptions:
- Big babies accept a college risk of their shoulders getting stuck (too known every bit shoulder dystocia).
- Big babies are at higher risk for other nativity problems.
- We can accurately tell if a baby volition exist big.
- Consecration keeps the infant from getting whatsoever bigger, which lowers the risk of Cesarean.
- Elective Cesareans for big baby are merely beneficial; that is, they don't have major risks that could outweigh the benefits.
Assumption #ane: Large babies are at higher chance for getting their shoulders stuck (shoulder dystocia).
Reality #ane: While it is true that 7-fifteen% of big babies have difficulty with the birth of their shoulders, near of these cases are handled by the care provider without any harmful consequences for the baby. Permanent nervus injuries due to stuck shoulders happen in i out of every 555 babies who weigh betwixt 8 lbs., 13 oz. and 9 lbs., xv oz., and 1 out of every 175 babies who weigh 9 lbs., xv oz. or greater.
1 of the main concerns with large babies is shoulder dystocia ("dis toh shah"). Shoulder dystocia is defined equally when shoulders are stuck enough that the care provider has to have extra physical action(s), or maneuvers, to assist get the baby out.
In the by, researchers take referred to shoulder dystocia equally the "obstetrician's greatest nightmare" (Chauhan 2014). The fear with shoulder dystocia is that it is possible that the babe might not become enough oxygen if the head is out only the trunk does not come out soon afterwards. In that location is likewise a risk that the baby will feel a permanent nerve injury to the shoulders.
Ane of the reasons that care providers take a fright of shoulder dystocia is because if the infant experiences an injury during or after shoulder dystocia, this type of injury is a common cause of litigation. In a study carried out at the University of Michigan, researchers plant that half of all parents whose children were being treated for shoulder dystocia-related injuries were pursuing litigation (Domino et al. 2014).
How oftentimes does shoulder dystocia occur? Researchers who combined results from 10 studies establish that shoulder dystocia happened to 6% of babies who weighed more than 4,000 grams (8 lbs., 13 oz.) versus 0.six% of those who were not big babies (Beta et al. 2019). When babies weighed more than 4,500 grams (ix lbs., 15 oz.), 14% experienced shoulder dystocia.
Similarly, one high-quality written report that looked separately at pregnant people with and without diabetes showed that in not-diabetic people, shoulder dystocia happened to 0.65% of babies who weighed less than viii lbs., xiii oz. (6.five cases out of i,000 births), 6.7% of babies who weighed betwixt 8 lbs., 13 oz. and ix lbs., 15 oz. (60 out of 1,000), and 14.5% of babies who weighed nine lbs., xv oz. or greater (145 out of one,000) (Rouse et al. 1996).
Rates of shoulder dystocia were much college in big babies whose birthing parent had Type I and Type Two diabetes (2.2% of babies that weighed less than 8 lbs., 13 oz., 13.9% of babies that weighed between 8 lb., 13 oz. and 9 lb., 15 oz., and 52.five% of babies that weighed more 9 lb., xv oz.) (Rouse et al. 1996).
We were not able to find verbal numbers for the percentage of people with gestational diabetes who had a baby with shoulder dystocia, as the rates change depending on each person's claret carbohydrate level. Even so, there is strong evidence that handling for gestational diabetes drastically lowers the chance of having a big infant and shoulder dystocia. We encompass the testify on handling for gestational diabetes (link evidencebasedbirth.com/inducingGDM) in our Evidence Based Nativity® Signature Article on Induction for Gestational Diabetes.
It'due south interesting to notation that people with loftier blood carbohydrate levels during pregnancy are at increased risk of shoulder dystocia during birth even when the baby is not big. This is because weight can be distributed differently on a infant when their gestational carrier has loftier blood sugars. Problems are more probable to occur if the baby'southward head size is relatively modest compared to the size of its shoulders and abdomen (Kamana et al. 2015).
Although large babies are at higher take chances for shoulder dystocia, at least half of all cases of shoulder dystocia happen in smaller or normal sized babies (Morrison et al. 1992; Nath et al. 2015). This is because overall, at that place are more small and normal size babies built-in than big babies. In other words, the rate of shoulder dystocia is college in bigger babies, but the absolute numbers are about the aforementioned with bigger and smaller babies. Unfortunately, researchers have found that information technology is impossible to predict exactly who will have shoulder dystocia and who will not (Foster et al. 2011).
Considering at least half of shoulder dystocia cases occur in babies that are not big, and we tin can't predict who volition take a shoulder dystocia, shoulder dystocia will ever be a possibility during childbirth. That is, the take chances can only exist eliminated if all babies are born by Cesarean. Considering requiring everyone to accept a Cesarean is unethical and impractical, it is of import for health care providers to train for the possibility of a shoulder dystocia.
Other resource on resolving shoulder dystocia:
- There are ways care providers tin can help prevent and manage a shoulder dystocia. For more than information, read this article on shoulder dystocia by Midwife Thinking.
- Click here for a PowerPoint from a shoulder dystocia training course from the United kingdom of great britain and northern ireland.
- Spinning Babies offers an online continuing instruction course nigh resolving shoulder dystocia. You tin also download a complimentary PDF on the FLIP-Flop technique for managing shoulder dystocia here.
- This video and this commodity draw how care providers can utilise a technique called the "shoulder shrug maneuver" to resolve shoulder dystocia (Sancetta et al. 2019).
- The Royal Higher of Obstetricians and Gynecologists has a guideline (last reviewed in 2017) on predicting, preventing, and managing shoulder dystocia hither.
Brachial plexus palsy
A shoulder dystocia by itself is not considered a "bad outcome." It's just a bad outcome if an injury occurs along with the shoulder dystocia (Personal communication, Emilio Chavirez, Medico, FACOG, FSMFM). Although nearly cases of shoulder dystocia tin be safely managed by a care provider during the nascency, some can result in a nerve injury in the baby called brachial plexus palsy.
Brachial plexus palsy, which leads to weakness or paralysis of the arm, shoulder, or hand, happens in about i.3 out of every 1,000 vaginal births in the U.S. and other countries. A baby does not take to take shoulder dystocia to feel a brachial plexus palsy—in fact, 48%-72% of brachial plexus palsy cases happen without shoulder dystocia. When a brachial plexus palsy happens at the same time equally shoulder dystocia, withal, it is more than probable to end up in a lawsuit than a brachial plexus palsy that did not occur with a shoulder dystocia (Chauhan et al. 2014).
Although rare, brachial plexus palsy can likewise happen to babies born by Cesarean. In i study that looked at 387 children who experienced brachial plexus palsy, 92% were built-in vaginally and viii% were built-in by Cesarean (Chang et al. 2016). Other researchers have found that brachial plexus palsy happens in virtually 3 per x,000 Cesarean births (Chauhan et al. 2014).
Some infants who take a brachial plexus palsy (about x%-18%) volition terminate upwards with a permanent injury, divers equally arm or shoulder weakness that persists for more a twelvemonth after birth. It'due south estimated that in that location are anywhere from 35,000 to 63,000 people living with permanent brachial plexus injuries in the U.S. (Chauhan et al. 2014). For a blog article nigh what it's like to grow up with a brachial plexus palsy, read Nicola's story hither.
In 2019, researchers combined five studies virtually the risks of brachial plexus injury in pregnancies with babies over eight lbs., 13 oz. versus those with babies who were not large (Beta et al 2019). Big babies had significantly more brachial plexus injury (0.74% versus 0.06%). When babies weighed more than than 4,500 grams (9 lbs., 15 oz.), the rate went up to 1.9%.
In a recent study of infants who were all extremely large at birth (>5000 g, or >xi lbs.), 17 of 120 infants born vaginally had shoulder dystocia, and three of those 17 had temporary brachial plexus palsy that healed within vi months—for an overall rate of about one brachial plexus palsy cases per xl vaginally-born, extremely big babies (Hehir et al. 2015).
In 1996, Rouse et al. published rates of shoulder dystocia and brachial plexus palsy by infant weight. Using the numbers of permanent inability published past Chauhan et al. in 2014, nosotros created a tabular array that helps show the difference betwixt the weight groups.

Importantly, research has shown that when health intendance professionals undergo almanac inter-professional person preparation (this means doctors, nurses, and midwives training together every bit a team) on how to handle shoulder dystocia, they can lower—and in some cases eliminate—brachial plexus palsy amid babies who experience shoulder dystocia (Crofts et al. 2016). Doctors take been trying to have this successful training (chosen "PROMPT") from the United Kingdom and implement it in the U.Southward. Results at the University of Kansas showed a decline and then an eventual emptying of permanent cases of brachial plexus palsy with PROMPT almanac trainings (Weiner et al. 2015).
To watch a news video most the PROMPT training, click hither. To visit the PROMPT foundation website, clickhttps://www.promptmaternity.org/.
Can a baby dice from shoulder dystocia?
Deaths from shoulder dystocia are possible just rare. In 1996, researchers looked at all the studies so far that had reported the rate of expiry due to shoulder dystocia. In xv studies, in that location were 1,100 cases of shoulder dystocia and no deaths (a decease rate of 0%). In two other studies, the rates of infant death were ane% (1 infant out of 101 "died at delivery," maybe due to the shoulder dystocia) and 2.five% (one baby died out of xl cases of shoulder dystocia) (Rouse et al. 1996).
In a study published by Hoffman et al. in 2011, researchers looked at 132,098 people who gave birth at term to a live baby in head- commencement position. Nigh one.5% of the babies had a shoulder dystocia (two,018 cases), and of those, 101 newborns were injured. Well-nigh of the injuries were brachial plexus palsy or collar bone fractures. Out of the 101 injured infants, there were zero deaths and half dozen cases of brain harm due to lack of oxygen. With the six encephalon-damaged infants, it took an average of 11 minutes between the birth of the head and the body.
Supposition #ii: Big babies tin can lead to a higher take chances of health problems and complications.
Reality #2: The risk of complications with a big baby increases along a spectrum (lower take chances at 8 lbs., 13 oz., higher risk at 9 lbs., 15 oz., and highest run a risk at 11+ lbs.). In addition, the care provider'south "suspicion" of a large baby carries its own prepare of risks.
Unplanned Cesareans
Researchers combined ten studies (chosen a meta-analysis) and plant that babies with nativity weights over 4,000 grams (8 lbs., 13 oz.) are more than likely to take labors that end in Cesarean (Beta et al. 2019). In these studies, the boilerplate Cesarean charge per unit was nineteen.3% for big babies versus xi.2% for babies who were not large. When babies weighed more than 4,500 grams (ix lbs., 15 oz.), the Cesarean rate increased to 27%. As we will hash out, a intendance provider's "suspicion" of a big baby can touch their likelihood of recommending Cesarean during labor.
Perineal Tears
In the meta-analysis published by Beta et al. (2019), five studies constitute a significant increase in the odds of severe tears with big babies, while 3 studies did not find a difference. When the researchers combined the results from all 8 studies, the overall result showed that those who give birth to large babies are more likely to have severe perineal tears, besides known equally third or fourth degree tears. The risk of a severe tear was ane.seven% when birthing big babies versus 0.nine% for birthing babies who were not large. When babies weighed more than than four,500 grams (9 lbs., 15 oz.), the charge per unit of severe tears was 3%.
The largest study (over 350,000 pregnant participants from National Health Service hospitals) examined 3rd degree tears and found the charge per unit to be 0.87% with big babies versus 0.45% without (Jolly et al. 2003). In this written report, pregnancies with big babies were also more likely to have longer offset and second stages of labor and more use of vacuum and forceps. The increase in the apply of vacuum and forceps amid big babies likely contributed to the increment in severe tears.
The 2nd largest study, which included over 146,000 hospital births in California betwixt 1995 and 1999, constitute a higher rate of 4th degree tears in large babies who were born vaginally (Stotland et al. 2004). However, 4th degree tear rates in this written report were very high, even among normal weight babies (i.5%), and the authors did not describe how many birthing people had episiotomies, which is a leading cause of astringent tears.
Although having a big baby may be a chance factor for severe tears, it may be helpful to compare this risk to other situations that can also increment the risk of tears. For instance, 1 big study found that the gamble of a severe tear with a big baby ranged from 0.ii% to 0.6% (Weissmann-Brenner et al. 2012).Other researchers have found that a vacuum delivery increases the risk of a astringent tear by 11 times. And then, if your baseline run a risk was 0.two%, it would increase to 2.2% with a vacuum, and the utilise of forceps increases the risk of a astringent tear by 39 times (from 0.2% to 7.8%) (Sheiner et al. 2005).
Postpartum Hemorrhage
Researchers combined nine studies that reported on postpartum hemorrhage in people who gave birth to big babies compared to those who birthed babies who were not big (Beta et al. 2019). They found a higher rate of hemorrhage with babies over eight lbs., 13 oz. (4.7% versus ii.3%). When the nativity weights were over 4,500 grams (9 lbs., 15 oz.), the charge per unit of postpartum hemorrhage was 6%. Yet, information technology is not clear whether this higher rate of postpartum hemorrhage is due to the big babies themselves or the inductions and Cesareans that care providers oftentimes recommend for a suspected large baby (Fuchs et al. 2013)—every bit both these procedures tin increment the run a risk of postpartum hemorrhage (Magann et al. 2005).
Newborn complications
One study compared 2,766 big babies with the same number of babies with normal nascency weights. All babies in the study were born to not-diabetic parents (Linder et al. The researchers found that big babies were more likely to have depression blood saccharide afterward birth (1.2% vs. 0.5%), temporary rapid animate (also known as "transient tachypnea" or "wet lung," 1.5% vs. 0.5%), high temperature (0.half dozen% vs. 0.one%), and birth trauma (2% vs. 0.seven%).
The researchers did not say whether intendance providers suspected that the babies were large before labor began, or if their care was managed differently. More of the large infants in this study were built-in past Cesarean (33% vs. 15%), which could have played a role in the higher rates of animate problems, since breathing issues are more common with Cesarean-born babies.
Birth fractures, or broken collar bones or artillery, are rare but more than likely to occur among big babies. Researchers combined the results from five studies and found that the rate of nativity fractures amongst babies over 4,000 grams (viii lbs., thirteen oz.) was 0.54% versus 0.08% amidst babies who are non big (Beta et al. 2019). When babies weighed more than 4,500 grams (9 lbs., 15 oz.), the fracture rate was increased to 1.01%.
Stillbirth
Some doctors recommend Cesareans for suspected big babies because they believe there is a higher risk of stillbirth.
In 2014, researchers published a written report where they looked dorsum in fourth dimension at 784,576 births that took identify in Scotland between the years 1992 and 2008. They included all babies who were born at term or mail service-term (between 37 and 43 weeks). They did not include multiples or any babies who died from congenital anomalies (Moraitis et al. 2014).
Babies in this written report were grouped according to their size for gestational age—fourth to 10th percentile, 11th to 20th percentile, 21st to 80th percentile (considered the normal grouping), 81st to 90th percentile, 91st to 97th percentile, and 98th to 100th percentile. The gestational age of each infant was confirmed by ultrasounds that took identify in the commencement half of pregnancy.
In this study, there were 1,157 stillbirths, and the hazard of stillbirth was highest in the groups with the smallest babies (1st to third and quaternary to 10th percentiles). The third highest take a chance of stillbirth death was seen in the babies who were in the 98th to 100th percentiles for weight (extremely large for gestational historic period). Using the American Academy of Pediatrics growth curve for gestational age, the 98th to 100th percentiles would be roughly equivalent to a babe who is built-in weighing 9 lbs., xv oz. or greater at 41 weeks.
Meanwhile, the lowest rates of stillbirth were in babies who were in the 91st to 97th percentiles. The increase in stillbirth gamble in the largest group (98th to 100th percentile) was partly explained by the birth parent being diabetic; however, there was also a higher gamble of unexplained stillbirth for babies in the 98th to 100th percentile. Overall, the absolute risk of an extremely large for gestational age baby (98th to 100th percentile) experiencing stillbirth between 37 and 43 weeks was almost 1 in 500, compared to 1 in ane,000 for babies who are in the 91st to 97th percentile.
Some other study on this topic looked dorsum in time at 693,186 births and 3,275 stillbirths between 1992-2009 in Alberta, Canada (Woods and Tang, 2018). They included all babies born at ≥23 weeks merely did not include multiples.
This big Canadian database study establish several risk factors for stillbirth: giving nascency for the start fourth dimension, having college body mass alphabetize (BMI), smoking in pregnancy, older historic period, and having medical problems earlier pregnancy such as high claret pressure level and diabetes. Like the previous study, pocket-sized for gestational age was a strong risk factor for stillbirth. But babies who were big for gestational age were not at whatever increased hazard for stillbirth. In fact, existence big for gestational age was protective against stillbirth in the full general population.
However, when researchers looked specifically at nativity parents with gestational diabetes, being large for gestational age was linked with a higher risk of stillbirth. The same was true for birth parents with Blazon I or Type II diabetes.
The run a risk of stillbirth has historically been higher in pregnant people with Type I or Type Two diabetes. However, in recent years the stillbirth rate for those with Type I or Type Two diabetes has drastically declined due to improvements in how diabetes is managed during pregnancy (Gabbe et al. 2012). Every bit far as gestational diabetes goes, the largest study ever done on gestational diabetes plant no link between gestational diabetes and stillbirth (Metzger et al. 2008). In the Canadian study, gestational diabetes was not linked with a higher risk of stillbirth unless the baby was also considered to exist large for gestational age.
In 2019, a large study in the U.South. analyzed medical records of stillbirths that occurred betwixt 1982 and 2017. The purpose of this study was to look at the possible relationship between big babies and stillbirth, but other factors were also considered (Salihu et al. 2014). It is important to note that overall, the rates of stillbirth have declined dramatically in both big and normal-sized babies over the last four decades. The decline in stillbirths may be due to advancements in medical training and pregnancy screening. In this study population, the rate of stillbirth in big babies declined 48.five% (from 2.04 per ane,000 to 1.1 per 1000), and information technology also declined 57.4% in babies of normal size (from ane.95 per 1,000 to 0.83 per 1000).
In total, more than 100 million pregnancies were analyzed in this study. About 10% of the full number of pregnancies were big babies. In the big infant group, in that location were 1.2 stillbirths per one,000 pregnancies, compared to i.ane stillbirths per i,000 pregnancies in the normal nascency weight range.
The researchers bespeak out that the risk of a big babe being stillborn varies from situation to state of affairs, and then care should be individualized. In other words, not all big babies acquit the same level of potential gamble when information technology comes to the chances of stillbirth. In their study, researchers separated the babies into 3 groups (form 1 or 4000-4499 grams, grade 2 or 4500-5000 grams, and grade three or over 5000 grams). Babies in the grade 3 group experienced an 11-fold increase in stillbirth (xi stillbirths per i,000 pregnancies) when compared to babies in the grade 1 grouping (1 stillbirth per 1,000 pregnancies). However, form 3 big babies fabricated up only 1.v% of the total big babe group, while grade one large babies made up more than 85% of the total big baby group. Overall, the grouping with the highest risk of stillbirth was the low birthweight group (14.89 stillbirths per ane,000 pregnancies). The 2nd highest rate of stillbirth was in the grade 3 big infant group. Some strengths of this report are the large data gear up and the classification of big babies into grades of macrosomia. A limitation is that considering of the mode the data was collected, we don't know if significant people who were diagnosed with "diabetes" had gestational diabetes or pre-existing Type one or Type 2 diabetes.
Is it Harmful to Suspect a Big Baby?
When a large baby is suspected, families are more than likely to feel a alter in how their care providers see and manage labor and birth. This leads to a higher Cesarean rate and a higher rate of people inaccurately being told that labor is taking "too long" or the babe "doesn't fit."
In fact, research has consistently shown that the care provider'south perception that a infant is large can be more harmful than an bodily big baby by itself.
have all shown that it is the suspicion of a big infant—non big babies themselves—that tin can atomic number 82 to college consecration rates, higher Cesarean rates, and higher diagnoses of stalled labor (Levine et al. 1992; Weeks et al. 1995; Parry et al. 2000; Weiner et al. 2002; Sadeh-Mestechkin et al. 2008; Blackwell et al. 2009; Melamed et al. 2010; Little et al. 2012; Peleg et al. 2015).
In one study, researchers compared what happened when people were suspected of existence pregnant with a big baby (>8 lbs., 13 oz.) versus people who were not suspected of being pregnant with a big baby—merely who concluded up having one (Sadeh-Mestechkin et al. 2008).
The cease results were amazing. Birthing people who were suspected of having a big babe (and actually concluded upward having one) had triple the consecration rate, more than triple the Cesarean charge per unit, and a quadrupling of the maternal complication rate, compared to those who were non suspected of having a big babe just had 1 anyway.
Complications were most frequently due to Cesareans and included bleeding (hemorrhage), wound infection, wound separation, fever, and need for antibiotics. In that location were no differences in shoulder dystocia between the two groups. In other words, when a care provider "suspected" a large babe (equally compared to non knowing the baby was going to be big), this tripled the Cesarean rates and fabricated mothers more than likely to experience complications, without affecting the rate of shoulder dystocia (Sadeh-Mestechkin et al. 2008).
These results were supported by some other study published past Peleg et al. in 2015. At their infirmary, physicians had a policy to counsel everyone with suspected big babies (suspected of being 8 lbs., 13 oz. and higher, or ≥4,000 grams) well-nigh the "risks" of large babies. Constituent Cesareans were non encouraged, but they were performed if the family requested one after the discussion. There were 238 participants who had suspected big babies (that concluded up truly being big at nativity) and were counseled, and 205 participants who had unsuspected big babies (that concluded upward existence truly large at birth) who were not counseled.
Even though the babies were all near the aforementioned size, only 52% of participants in the suspected big babe group had a vaginal birth, compared to 91% of participants in the not-suspected large baby grouping. This increase in Cesarean rate in the suspected big baby group was primarily due to an increase in the families requesting elective Cesareans after the "counseling" session almost how big babies are risky to birth. There was only ane instance of shoulder dystocia in the unsuspected big baby group, and ii cases in the suspected big baby grouping. None of these babies experienced injuries. There was no difference in severe birth injuries between the 2 groups.
The authors concluded that obstetricians should not exist counseling pregnant people virtually the risks of large babies thought to be 8 lbs. 13 oz. or higher, because it leads to an increase in the number of unnecessary Cesareans without any benefit to the birthing person or baby. They suggested that researchers should study using a college weight cut-off (such as ix lbs., fifteen oz.) to trigger counseling.
Other researchers accept found that when a start-time parent is incorrectly suspected of having a large baby, intendance providers take less patience with labor and are more likely to recommend a Cesarean for stalled labor. In this study, researchers followed 340 starting time-time birthing people who were all induced at term. They compared the ultrasound approximate of the baby's weight with the actual birth weight. When the ultrasound incorrectly said the baby was going to weigh more than than 15% higher than it ended up weighing at birth, physicians were more than twice as likely to diagnose "stalled labor" and perform a Cesarean for that reason (35%) than if there was no overestimation of weight (thirteen%) (Blackwell et al. 2009b).
Pregnant people who are plus size and those who accept medication for high blood carbohydrate likewise experience an increase in unplanned Cesareans when ultrasound is used to estimate the babe's weight (Dude et al. 2019; Dude et al. 2018).
A recent study from the U.Southward. looked at ii,826 first-fourth dimension birthing people with a body mass index (BMI) ≥ 35 kg/mtwo (Dude et al. 2019). Out of everyone in the study, 23% had an ultrasound to estimate the babe'south weight inside 35 days of birth. The participants who had an ultrasound to estimate the infant's weight were more than likely to have an unplanned Cesarean (mostly for "stalled labor") than those without an ultrasound-estimated fetal weight (43% versus thirty%). Having an ultrasound to estimate the baby's weight was linked with a higher rate of Cesarean even later on considering other factors that could have impacted the Cesarean rate, including the baby's bodily birth weight.
Amongst the 636 participants who had an ultrasound to estimate the baby's weight, 143 of them were told that their babies were big for gestational historic period (measuring over the xcthursday percentile). This group had a much higher rate of Cesarean (61% versus 31%). Even so, only 44% of them (61 out of the 143 birthing people) gave birth to a babe that was large for gestational historic period.
The authors found similar results when they looked at effectually 300 people who were giving birth for the first time and taking medication for high claret sugar (Dude et al. 2018). Again, having an ultrasound to guess the baby'due south weight within 35 days of birth was linked to a higher charge per unit of unplanned Cesareans (52% for those with an ultrasound versus 27% for those without an ultrasound) fifty-fifty afterward considering the baby'southward actual birth weight and other medical factors.
The authors conclude, "Perceived knowledge of fetal weight may affect decisions providers brand regarding how likely they feel their patients are to deliver vaginally."
It'south not surprising that physicians are more likely to plough to Cesarean in these situations, given a cultural fear of big babies. In i medical journal editorial, an obstetrician with a clear bias towards Cesarean for large babies said that, "Flagging up all cases of predicted fetal macrosomia is vitally important, and then that the attendants in the labor suite will recommend Cesarean if there is any delay in cervical dilatation or abort of head rotation or descent. Cesarean should also be the preferred pick if an aberrant fetal centre tracing develops" (Campbell, 2014).
So, in summary, although large babies are at higher risk for some problems, the care provider'due south perception that at that place is a big babe carries its own set of risks. This perception—whether it is true or false—changes the style the care provider behaves and how they talk to families virtually their ability to birth their baby, which, in plow, increases the hazard of Cesarean.
Assumption #3: We can tell which babies will be big at nascence.
Reality #3: Both physical exams and ultrasounds are as bad at predicting whether a baby volition be big at nativity.
Time and time once more, researchers take found that it is very difficult to predict a infant'south size before it is born. Although two out of iii people giving nascence in the U.S. receive an ultrasound at the end of pregnancy (Declercq et al. 2013) to "estimate the infant's size," both the care provider's estimate of the baby's size and ultrasound results are unreliable.
In 2005, researchers looked at all the studies that had always been washed on ultrasound and estimating the baby's weight at the end of pregnancy. They found 14 studies that looked at ultrasound and its ability to predict that a baby would weigh more than 8 lbs., 13 oz. Ultrasound was authentic xv% to 79% of the time, with most studies showing that the accurateness ("mail-test probability") was less than l%. This ways that for every 10 babies that ultrasound predicts volition weigh more than than 8 lbs., 13 oz., 5 babies will weigh more that and the other v will counterbalance less (Chauhan et al. 2005).
Ultrasound was even less accurate at predicting babies who will exist born weighing nine lbs., 15 oz. or greater. In three studies that were washed, the accuracy of ultrasounds to predict extra-large babies was only 22% to 37%. This means that for every 10 babies the ultrasound identified as weighing more than than ix lbs., xv oz., simply ii to 4 babies weighed more than this amount at nascency, while the other six to eight babies weighed less (Chauhan et al. 2005).
The researchers found 3 studies that looked at the ability of ultrasound to predict big babies in pregnant people with diabetes. The accurateness of these ultrasounds was 44% to 81%, which ways that for every ten babies of a diabetic parent who are thought to weigh more than eight lbs., xiii oz., around vi will counterbalance more and 4 will weigh less. The ultrasound examination probably performs better in diabetics merely because diabetics are more likely to have big babies. In other words, it'southward easier to predict a large infant in someone who is much more likely to have a large baby to begin with.
Currently, there is no reason to believe that three-dimensional (3D) ultrasound is any ameliorate at predicting nativity weight and large babies than ii-dimensional (second) ultrasound (Tuuli et al. 2016). Research is ongoing to determine if 3D measurements tin be combined with second measurements to better predict macrosomia.
There is also no show that magnetic resonance imaging (MRI) improves the accuracy of fetal weight estimates. The kickoff prospective clinical report to compare estimated fetal weight from 2nd ultrasound versus MRI is currently being conducted in Belgium (Kadji et al. 2019). The researchers recollect that MRI at 36 to 37 weeks of pregnancy could be much more accurate than ultrasound at predicting large babies. Nevertheless, even if MRI is found to be superior, information technology is very expensive and probably not practical.
Compared to using ultrasound, care providers are just as inaccurate when it comes to using a physical exam to estimate the size of the baby. However, ultrasound appears to provide more accurate estimates when pregnant people are plus size (Preyer et al. 2019).
Overall, when a care provider estimates that a baby is going to weigh more than 8 lbs., 13 oz., the accuracy is just twoscore-53% (Chauhan et al. 2005). This ways that out of all the babies that are thought to counterbalance more than 8 lbs., 13 oz., half will weigh more than than eight lbs., xiii oz. and half volition weigh less.
The care provider's accurateness goes up if the pregnant person has diabetes or is post-term, once again, probably considering the take chances of having a big infant is higher amidst these groups. Unfortunately, all the studies that looked at diabetes and the accuracy of ultrasound lumped people with gestational diabetes and those with Type I or Blazon Two diabetes into the aforementioned groups, limiting our power to interpret these results.
A systematic review ended that at that place is "no clear consensus with regard to the prenatal identification, prediction, and management of macrosomia." The authors stated that the main trouble with big babies is that it is very hard to diagnose large babies earlier birth—it's a diagnosis that tin can only exist made after birth (Rossi et al. 2013).
Even the "best" way to predict a big baby is going to take bug identifying actual big babies—nearly often overestimating the size of the baby. In a 2010 study past Rosati et al., researchers tested dissimilar ultrasound "formulas" to figure out an infant's estimated weight. The best formula for predicting nativity weight was the "Warsof2" formula, which is based solely on the baby's abdominal measurement. The results of this formula came within ±xv% of the infant's actual weight in 98% of cases. As an example, if your baby's actual weight was 8 lbs. (3,629 grams), the ultrasound could guess the infant's weight to exist anywhere between 6 lbs., 13 oz. (3,090 grams) and 9 lbs., 3 oz. (4,450 grams).
Many weight interpretation formulas have been published (new 2d and 3D formulas are added every yr), and researchers continue to debate whether they are accurate.
Recently, a study compared the "Hart" weight estimation formula to the "Hadlock" formula (Weiss et al. 2018). The "Hadlock" formula is very popular today and considered by many to exist the most accurate (Milner and Arezina, 2018). Weiss et al. institute that compared to the "Hadlock" formula, the "Hart" formula greatly overestimated fetal weight when babies weighed less than viii lbs., 13 oz. (4,000 grams) and failed to detect very large babies. The authors expressed concern that using the "Hart" formula could lead to an increased charge per unit of labor consecration and Cesareans, and they concluded that it has no place in clinical practice.
Supposition #4: Consecration allows the baby to be born at a smaller weight, which helps avert shoulder dystocia and lowers the run a risk of Cesarean.
Reality #four: At that place is conflicting testify almost whether consecration for suspected big babies tin can improve health outcomes.
We will talk nearly three main pieces of evidence in this section:
- A 2016 Cochrane review (when researchers combined multiple randomized trials together)
- The largest written report (published in 2015) from the Cochrane review
- The 2d-largest study (published in 1997) from the Cochrane review
Cochrane Review
In a 2016 Cochrane review, researchers (Boulvain et al. 2016) combined four studies in which 1,190 non-diabetic pregnant people with suspected large babies were randomly assigned (like flipping a money) to either ane) induction between 37 and 40 weeks or two) waiting for spontaneous labor.
When researchers compared the consecration group to the waiting group, they establish a decrease in the rate of shoulder dystocia in the induction grouping—almost 41 cases per 1,000 births in the elective induction grouping, downwardly from 68 cases per one,000 in the waiting grouping.
They also establish a decrease in birth fractures in the elective induction grouping (4 per 1,000 vs. xx per ane,000 in the waiting group). To forbid one fracture, it would be necessary to induce labor in 60 people.
On the other hand, they plant an increase in astringent perineal tears in the induction group (26 per one,000 in the induction group vs. 7 per 1,000 in the waiting group), as well as an increase in the handling of jaundice (11% vs. vii%).
On average, babies weighed 178 grams (6 ounces) less when labor was electively induced, compared with those assigned to wait for labor.
There were no differences between groups in rates of Cesarean, instrumental delivery, NICU admissions, brachial plexus palsy, or low Apgar scores. Three of the four studies reported death rates, and there were zero deaths in either group.
Researchers did not look at patients' satisfaction with their care or any long-term health results for birthing people or babies.
Largest report in Cochrane review (2015)
The study published by Boulvain et al. 2015 was the largest study in the Cochrane review. In this written report, researchers followed 818 pregnant people with suspected big babies who were randomly assigned to either a) induce labor betwixt 37 to 38 weeks, or b) expect for labor to start on its own until 41 weeks. This is the largest randomized trial that has always been done on consecration for suspected big babies.
Pregnant people could exist in the study if they had a unmarried baby in head-down position, whose estimated weight was in the 95th percentile (>7 lbs., eleven oz. at 36 weeks, 8 lbs., three oz. at 37 weeks, or 8 lbs., ten oz. at 38 weeks). About 10% of the participants in this study had gestational diabetes.
In that location was some cross-over between groups: 11% of participants in the induction group went into labor on their own, and 28% of participants in the waiting-for-labor group were induced.
The researchers found that pregnant people randomly assigned to the induction group (whether or not they were really induced) had fewer cases of shoulder dystocia: one% of people in the induction group (v out of 407) had true shoulder dystocia compared with 4% (16 out of 411) of those in the expectant management group. None of the babies in either group experienced any brachial plexus palsy injuries, and collarbone fracture rates were low in both groups (ane to 2%).
The chances of having a spontaneous vaginal birth was slightly more mutual in the induction group (59% vs. 52%), but in that location was no difference in the rates of Cesarean and the apply of forceps or vacuum. There were no other differences in birth outcomes, including any tears or hemorrhage.
The infants in the induction group were more probable to accept jaundice (9% vs. three%) and receive phototherapy treatment (11% vs. 7%). There were no differences in NICU admission rates or any other newborn differences between groups.
In summary, this study constitute that early consecration (at 37-38 weeks) lowered the rate of shoulder dystocia, simply without whatever accompanying affect on actual brachial plexus palsy rates, collarbone fractures, or NICU admissions.
The authors suggested that the main reason they establish dissimilar results from an earlier randomized trial by Gonen et al. (1997), is because they checked fetal weight before and induced babies earlier— betwixt 37 to 39 weeks, instead of waiting until 38 to 39 weeks. This meant that they induced labor when a fetus is large for gestational age, but before it was technically "big," resulting in the nativity of a normally sized baby a few weeks early. For example, in the Gonen et al. written report discussed adjacent, pregnant people were not included in the study until they were at least 38 weeks meaning and their estimated fetal weight reached 8 lbs., xiii oz. Meanwhile, in the newer trail past Boulvain et al., of the 411 infants in the waiting-for-labor group, 62% weighed more than than 4000 g (8 lbs., thirteen oz.) at birth, compared with 31% of those who were induced. This ways that the participants who waited for labor to starting time on its own ended upward with large babies, while those who were induced early gave birth earlier their babies could go large.
The authors of the Boulvain written report remember that previous studies have non institute a benefit to consecration because providers waited likewise long to arbitrate, and they missed their chance for the mother to birth a smaller baby and reduce the risk of shoulder dystocia. Although this approach—inducing labor between 37 and 39 weeks—resulted in lower rates of shoulder dystocia, information technology also led to college rates of newborn jaundice, and it did not take whatever bear on on "difficult" outcomes such as brachial plexus palsy or NICU admission.
Second-largest study in the Cochrane Review
The Gonen et al. (1997) study was the 2nd-largest study in the Cochrane review (with 273 participants). In this written report, significant people were included if they were at to the lowest degree 38 weeks, had a suspected large babe (eight lbs., 13 oz. to 9 lbs., 15 oz.), did not have gestational diabetes, and had not had a previous Cesarean. Less than one-half the participants were giving birth for the start time. Participants were randomly assigned to either immediate induction with oxytocin (sometimes also with cervical ripening) or waiting for spontaneous labor.
The results? Participants in the spontaneous labor group went into labor virtually five days subsequently than those who were immediately induced. Although participants in the spontaneous labor group tended to have slightly bigger babies (on boilerplate, 3.v oz. or 99 grams heavier), there was no difference in shoulder dystocia or Cesarean rates. All xi cases of shoulder dystocia, spread across both groups, were easily managed without any nerve harm or trauma. Two infants in the waiting-for-labor group had temporary and mild brachial plexus palsy, just neither of these ii infants had shoulder dystocia. Finally, ultrasound overestimated the babe'south weight lxx% of the fourth dimension and under-estimated the baby's weight 28% of the time.
In summary, the researchers found that: 1) ultrasound estimation of weight was inaccurate, 2) shoulder dystocia and nerve injury were unpredictable, and 3) induction for large baby did non decrease the Cesarean rate or the risk of shoulder dystocia.
Supposition #five: Elective Cesarean for big infant has benefits that outweigh the potential harms.
Reality #5: No researchers have ever carried out a written report to determine the effects of elective Cesareans for suspected big babies.
Although some care providers will recommend an induction for a large baby, many skip this stride and go straight to recommending an elective Cesarean. All the same, researchers have estimated that this blazon of approach is extremely expensive and that it would take thousands of unnecessary Cesareans to prevent one instance of permanent brachial plexus palsy.
In 1996, an important analysis published in the Periodical of the American Medical Association proposed that a policy of elective Cesareans for all suspected large babies was non cost-constructive and that there were more than potential harms than potential benefits (Rouse et al. 1996).
In this analysis, the researchers calculated the potential effects of three different types of policies:
- No routine ultrasounds to estimate the babies' sizes
- Routine ultrasounds, so elective Cesarean for babies weighing 8 lbs., 13 oz. or more
- Routine ultrasounds, then constituent Cesarean for babies weighing nine lbs., 15 oz. or more
The researchers looked at the results separately for diabetic and not-diabetic people. Unfortunately, most research up to this time indicate did non distinguish between Type 1 or Blazon II diabetes and gestational diabetes. And then the term "diabetic" could refer to all three types.
Among non-diabetics, a policy of elective Cesarean for all suspected large babies over 8 lbs., thirteen oz. means that a large number of pregnant people and babies would experience unnecessary surgeries. In society to foreclose one permanent brachial plexus palsy in babies suspected to be over 8 lbs., thirteen oz., two,345 people would have unnecessary Cesareans at a cost of $iv.ix one thousand thousand dollars per injury prevented (costs were estimated using twelvemonth 1995 dollars).
With a policy of elective Cesareans for all suspected large babies over 9 lbs., fifteen oz., fifty-fifty more pregnant people would have surgeries found to be unnecessary in retrospect, because ultrasounds are even less accurate in higher suspected weight ranges (Chauhan et al. 2005). In order to preclude ane permanent brachial plexus palsy in babies suspected to be over 9 lbs., fifteen oz., three,695 people would need to undergo unnecessary Cesareans at a cost of $eight.vii meg per injury prevented.
Such policies would increase rates of known risks from Cesarean, similar serious infections, claret clot disorders, postpartum bleeding (hemorrhage) requiring claret transfusions, and newborn animate bug (run across "" from ChildbirthConnection.org).
Among diabetics, the results were unlike—mostly considering ultrasound is slightly more reliable at predicting large babies in meaning people who are diabetic, and considering shoulder dystocia is more than common in this group as well. If meaning diabeticswere offered an constituent Cesarean for every baby that is suspected of weighing more than viii lbs., xiii oz., information technology would take 489 unnecessary surgeries to prevent one example of permanent nerve damage, at a toll of $930,000 per injury avoided. If diabetics had elective Cesareans when their babies were suspected of existence 9 lbs., fifteen oz. or greater, it would have 443 unnecessary surgeries to prevent one case of permanent brachial plexus palsy, at a toll of $880,000 per injury avoided.
Please note: A cost-effectiveness analysis is but as practiced equally its assumptions–the numbers that they use to plug into the analysis. For example, how did they make up one's mind how frequently shoulder dystocia occurs, the accuracy of ultrasounds, and how many permanent injuries occur? In the Rouse et al. (1996) paper, the authors did a very high-quality literature review to determine these factors. One drawback of this analysis is that the costs they reported did not include the cost of lawsuits.
Another of import drawback is that this analysis is now over xx years old.
Since the landmark Rouse et al. paper was published, two newer cost-effectiveness analyses have been published. However, both of these newer papers had major problems—one of them did not take into account the inaccuracy of ultrasound (Herbst, 2005), and the other researchers had a poor-quality systematic review—using numbers in their assumptions that overestimate the accuracy of ultrasound (Culligan et al. 2005). Because the researchers did non do a adept job of making their assumptions, nosotros cannot trust the results of their analyses, and then their results are non included in this Signature Article.
In summary, bear witness does not support elective Cesareans for all suspected big babies, especially among non-diabetic pregnant people. There accept been no randomized, controlled trials testing this intervention for big babies, and no high-quality research studies to come across what happens when this intervention is used on a mass-scale in existent life.
In fact, significant people without diabetes may be given one-sided information past their care providers if elective Cesarean is presented as a completely "safe" or "safer" pick than vaginal nascence for a suspected large babe. Although vaginal birth with a big babe carries risks, Cesarean surgery also carries potential harms for the birthing person, infant, and any children built-in in future pregnancies. It is of import to have full information on both options in order to make a decision. To read more than near the potential benefits and harms of Cesarean versus vaginal birth, you may desire to read: "Vaginal or Cesarean Birth: What is at Stake for Women and Babies?" or the consumer booklet, "What every woman should know nearly Cesarean Section" from Childbirth Connexion.
Guidelines
In 2016, the American Congress of Obstetricians and Gynecologists (ACOG) released an opinion stating that induction is not recommended for suspected large babies, because consecration does not improve outcomes for birthing people or babies (recommendation based on "Level B testify = limited or inconsistent evidence"). The 2016 do bulletin was reaffirmed by ACOG in 2018. This recommendation is similar to their 2002 guidelines that were reaffirmed in 2008 and 2015, and somewhen replaced by this new position statement published in 2016. In 2020, ACOG released another practise bulletin stating that more inquiry needs to be done to determine whether the potential benefits of inducing for a suspected big infant to prevent shoulder dystocia before 39 weeks outweigh the risks of early on consecration (ACOG, 2020).
In 2008, the National Institutes for Health and Clinical Excellence (Overnice) in the Great britain likewise An updated recommendation from Overnice, released as a draft in May 2021, suggests that all pregnant people should be offered induction at 41 weeks, rather than assuasive babies to grow for upwards to 42 weeks, to lower possible complications. This advice is not specific to suspected big babies and is based on expert stance not clinical trials.
French practice guidelines from 2016 recommend induction for suspected big baby if the cervix is favorable at 39 weeks of pregnancy or more (Sentilhes et al. 2016). This recommendation is based on "professional consensus," not enquiry testify.
In all their opinion statements since 2002, ACOG has stated that planned Cesarean to forbid shoulder dystocia may be considered for suspected large babies with estimated fetal weights more than 11 lbs. (5,000 grams) in birthing people without diabetes, and ix lbs., xv oz. (4,500 grams) in birthing people with diabetes.. They state the evidence is "Grade C," meaning this recommendation is based on consensus and skilful opinion only, non inquiry bear witness (ACOG 2002; ACOG 2013; ACOG 2016—Reaffirmed French guidelines on elective Cesarean for suspected big babe are consistent with the ACOG recommendation.
Source: https://evidencebasedbirth.com/evidence-for-induction-or-c-section-for-big-baby/
0 Response to "What Is a Baby Called That Died Right Before Birth"
Post a Comment